FELLOWSHIP COLLABORATION OPPORTUNITIES
EM RESIDENT SIMULATIONS
The Simulation Fellows, with oversight from the Directors, are responsible for writing, implementing, and debriefing EM cases for resident didactic sessions at all four Simulation Collective Sites. This provides quadruple the teaching opportunities! Cases focus on EM skills and resuscitation, and help develop the residents into well rounded EM doctors.
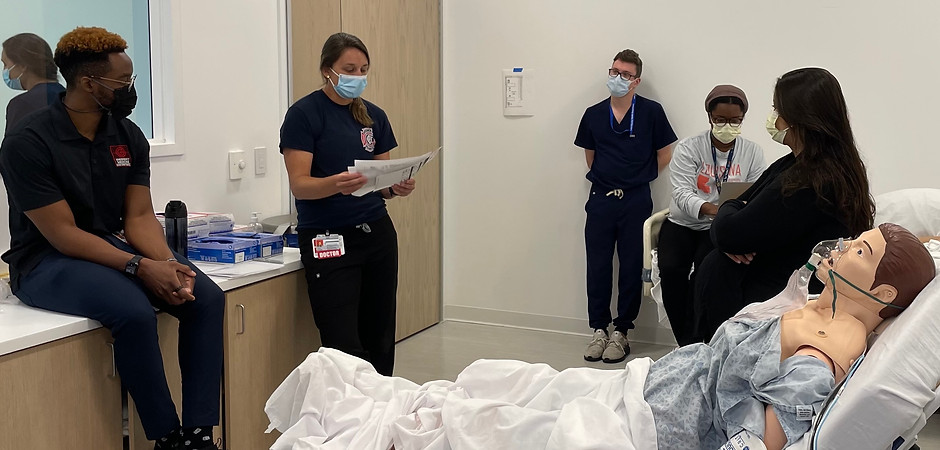
NON-EM SIMULATIONS
With four centers at which to teach, the opportunities are extensive. The Simulation centers operate to serve the following groups: Nursing, Internal Medicine, Family Medicine, Pediatrics, Medical ICU, General Surgery, Ophthalmology, Surgical ICU, Radiology, Anesthesia, OB/Gyne, Midlevel Providers, Trauma Surgery, Palliative Care, Paramedic Students, and ACLS/BLS/PALS Training, and many more.

MEDICAL STUDENT SIMULATIONS
Medical student simulations are also led by the simulation fellows, with emergency cases designed to be introductory to emergency medicine concepts and case management. Medical students planning on any field of study can participate in the simulations.

MONTHLY ACADEMIC DAY
A monthly group discussion, led by the 4 site directors, in which the fellows review important articles and innovations in simulation literature. Guest lectures from fellowship alumni provide a perspective of simulation-based medical education from multiple institutions.

DIVERSITY AT CCH SIMULATION CENTER
Lead by Dr. Ashlea Winfield - Strengthening the Pipeline - Using Simulation to Close Gaps for URiM Learners. Over the years the CCH Simulation Center has partnered with local nonprofits, high schools, and regional SNMA (Student National Medical Association) chapters to provide exposure to careers in emergency medicine for Chicago youth from historically excluded backgrounds.



SIMTASTIC
An annual event held among the emergency medicine residencies in the Chicago area, 2nd year EM residents join another institution for a fresh and fair-minded simulation assessment by the institution's simulation faculty.
Salzman D, Watts H, Williamson K, Sergel M, Dobiesz V, DeGarmo N, Sharp L, Wang E,
Gisondi M.“A Multicenter Collaboration for Simulation-Based Assessment of
ACGME Milestones in Emergency Medicine” Sim Healthcare 00:00–00, 201

RESUSCITATION AND PROCEDURE COURSES
Throughout the academic year, procedure courses and adult and pediatric resuscitation courses are held for the EM residents at all 4 sites of the Chicago Simulation Fellowship Collaboration.
NATIONAL CONFERENCE INVOLVEMENT
International Meeting on Simulation in Healthcare (IMSH)
Fellows are funded to attend the annual International Meeting on Simulation in Healthcare.
Rocky Mountain EM Conference
https://RockyMtnCME.com/
Under the guidance of Dr. Michelle Sergel, fellows will have the opportunity to participate in the
simulation and procedural workshops offered at this fun annual national conference in the Rocky Mountains - plenty of skiing available!
American College of Emergency Physicians (ACEP)
When opportunities arise for teaching and participating in lectures, workshops, and/or presentations, fellows will be allowed the opportunity to go to the ACEP.
Society for Academic Emergency Medicine (SAEM)
When opportunities arise for teaching and participating in lectures, workshops, and/or presentations, fellows will be allowed the opportunity to go to SAEM.

SIM WARS
Sim Wars is a fun-spirited contest of resuscitation simulations held at national conferences. Using a single elimination bracket, the winning team progresses through to the championship case. Team scores are based on medical knowledge, team work, procedural skills, and team spirit! The program directors are on the national Sim Wars planning committee and provide opportunities for the fellows to continue this fun tradition on a national level.

BOSTON COMPREHENSIVE INSTRUCTOR WORKSHOP:
CENTER FOR MEDICAL SIMULATION
Fellows will receive the opportunity to go to the intensive immersion in healthcare simulation course led by experienced simulation educators from Harvard Medical Center. It covers all high-level elements and concepts involved in running a simulation program. Depending on the fellowship site, this 5-day program in Boston, Massachusetts will be funded, including costs for airfare and lodging. The course focuses on:
-
Operating a simulation program
-
Developing debriefing skills
-
Preparing, building, conducting, and debriefing realistic simulation scenarios
-
Avoiding simulation pitfalls
-
Advancing simulation within one’s institution
Visit https://harvardmedsim.org/ims-comprehensive-workshop.php for more information.

SCHOLARSHIP PROJECTS
Each Fellow will select a Simulation-based Education (SBE) program or question to study.
Examples include:
-
Developing, piloting, and evaluating a new simulation-based educational program.
-
Evaluating an existing SBE program
-
Comparing two SBE programs, or SBE programs using alternative instructional or assessment methods.
-
Gathering evidence for the validity of an SBE assessment.
CCH, NorthShore/U of C, Rush and Loyola Simulation faculty will provide weekly mentorship and supervision of scholarship activities. Fellows are encouraged to disseminate their work via posters and presentations at national meetings, as well as submissions to MedEdPortal or PubMed indexed journals.
An administrative project is encouraged within the year of the fellowship. Due to the relatively new use of simulation-based medical education, simulation centers, labs, and programs are emerging regularly. The fellow should be prepared for future opportunities involving the creation of a new simulation center or improving upon a center (examples of administrative projects include website improvement/design, staff training/hiring, organization of materials or scheduling, etc.)
Summary of Criteria for Successful Fellowship Completion
-
Participation in most Simulation weekly activities (approximately 20 hours/week)
-
Scholarly project completion
-
Administrative project completion

LUC Stritch School of Medicine M3 Capstone OSCE
With the end of the Step 3 Clinical Skills exam, the Stritch School of Medicine was looking for a way to assess students at the end of the M3 year. Our fellow took an active role in designing an OSCE experience with Stritch School of Medicine leadership. The OSCE was designed with 3 clinic-setting simulation encounters with standardized patients, where one of those patients goes on to require resuscitation in the ED, using our high-fidelity simulation center and manikins. We assess the students and use this information to identify lower-performing students to give additional support during their M4 year.
LUC Stritch School of Medicine Simulation Elective
Simulation faculty have developed and are preparing for the first-ever simulation elective rotation at the Stritch School of Medicine for the fall of 2024. Through this course, students will explore their own career passions in various medical specialties by designing, running, and debriefing their own simulation cases. They will further their skills in teaching to help jump-start their careers in medical education and delve into the ever-evolving world of simulation.
LUMC Emergency Medicine Residency In-Situ Code Curriculum
In collaboration with Emergency Medicine residency faculty and nursing, simulation faculty are designing a formal curriculum of in-situ simulation cases for all levels of residents (PGY1-3), focusing on various arrest scenarios to be run in the Emergency Department. These scenarios offer hands-on education for various teams, increasing their knowledge and capabilities to manage both common and uncommon arrest scenarios. Residents specifically will further their departmental awareness, communication, and
team management skills when participating in these cases on shift.
LUMC Emergency Medicine Faculty Development in Simulation
Simulation faculty have designed educational materials with a specific focus on simulation case design and post-simulation debriefing tools for faculty to learn in a self-directed manner. Pre- and post-learning along with the utilization of techniques will then be assessed to help discern areas in need of improvement to further the overall capabilities of our simulation educators.
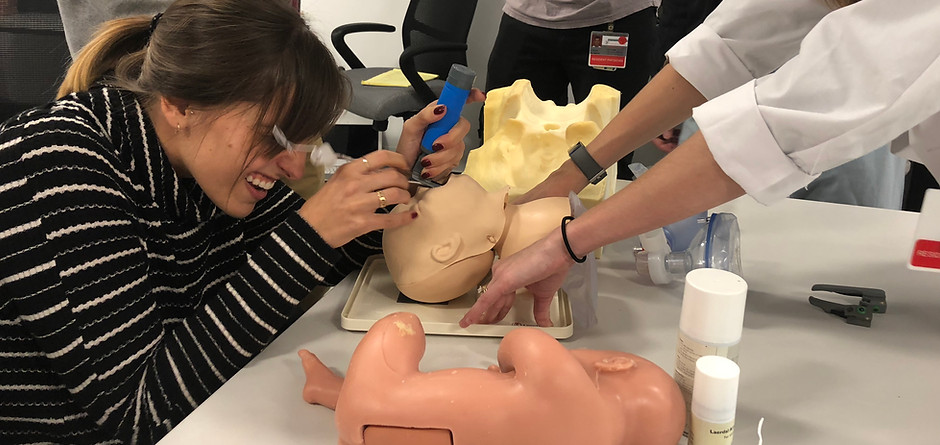
LUMC Neonatal Simulation
Simulation faculty have helped design and assess two neonatal simulation projects. Each of these projects has separately received a $5,000 York Educational Grant through the Department of Medical Education at Loyola University Stritch School of Medicine. One project is titled: “Rapid Cycle Deliberate Practice vs Traditional Simulation Education in Improving Residents’ Neonatal Resuscitation Skills Proficiency” and the other is titled: “Development and Evaluation of a Neonatal Simulation Curriculum for Community Hospitals Utilizing Rapid Cycle Deliberate Practice.”
The Simbulance Community Outreach
Simulation staff and faculty are collaborating with various community health initiatives in the north shore and beyond by using the Simbulances to bring simulation manikins and task trainers to help teach and emphasize specific health goals within those
communities. Various projects include BLS, hypertension, and diabetes training.
Clinical 3D Printing
In collaboration with NorthShore Cardiology, the NorthShore Sim Lab is creating 3D prints of patients’ hearts to help properly size the patient for specific intracardiac devices. This has led to decreased intraoperative time as well as less medical waste.
Projects are also being developed with other specialties such as Interventional Neurology and Orthopedics.
NorthShore In-Situ Training
Since NorthShore is a multi-hospital system, the sim lab is often called upon to do in-situ simulations at each hospital site. These are inter-professional as well as inter-disciplinary scenarios to help experience new protocols/locations or to identify latent safety threats. Using the Simbulances also helps bring the sim lab to all the hospitals without compromising on fidelity due to distance. Current in-situ projects include stroke and trauma simulations with more on the horizon.
